Julia Scoles was a top recruit and the 2016 ACC Freshman of the Year for the University of North Carolina indoor volleyball team when her life was derailed by a string of concussions. Her injuries forced her to transfer schools, change sports, and redefine herself. In this personal story, she vividly describes how she went from not taking concussions seriously, to suffering with Post-Concussion Syndrome (PCS), and having her symptoms impact every aspect of her life. Scoles originally shared her story with VolleyballlMag in 2019 and has updated it here for the Concussion Legacy Foundation to share her progress and new found passion as a beach volleyball player.

Posted: July 27, 2020
August 2019:
In the past two years, everything I once knew about my life changed. I was left in an ominous, dark place. My vibrant world shattered, and I’ve been trying to put the pieces together since. The cause of these life-altering circumstances? Concussions.
Before experiencing one of my own, the word “concussion” carried little weight. I had no awareness of the magnitude and severity a concussion could potentially have. At the time, I only knew of people experiencing minor concussions which seemed to have little to no impact on their actual life.

I hate to admit this, but I viewed players that didn’t practice or compete in their sport due to a concussion-related injury as somewhat undedicated — or even mentally weak. Growing up in athletics, I was taught to push through physical pain unless the injury was serious. Unlike other serious injuries, concussions are not visible, so understandably I viewed them as less significant. I thought having a concussion just meant that you would experience some headaches, a little light sensitivity, and that you were “supposed” to rest/not practice for a couple of days.
Boy, was I wrong.
It took having three concussions for me to finally understand the severity and detrimental effects concussions can have.
I received my first concussion during volleyball practice my freshman year at the University of North Carolina. We were doing a drill called “pit.” In the pit drill, one player is on the court at a time, going all out after each ball, which is hit at every imaginable speed and angle. Normally, the player digs a hard-driven hit or flails to pick up low shots. During the play where I got concussed, my coach tossed a ball fairly high down the line. I could have easily run there to play the ball on my feet without having to dive. However, in the most un-volleyball like manner, I took two steps to the corner, turned my body to the ball, and launched myself in its direction. I was parallel to the ground, at least three feet in the air, resembling the form of a perfect pool day “belly flop.”

Gravity took it from there and my face broke the fall. My teeth hit first (which I would later need orthodontic work to fix), then my nose, and lastly my forehead. I blacked out. The next thing I remember was waking up feeling liquid streaming down my face. I was confused and in pain. For some reason, I was determined to prove I wasn’t crying, so I announced to the circle of teammates surrounding me, “I promise I’m not crying,” to which someone quickly responded, “it’s blood, not tears.”
By this point, the athletic trainers were by my side to bring me off the court. I was completely out of it. Every time the trainers attempted to stand me up, my body would go limp and I would start to pass out.
The pain didn’t start to kick in until I was placed in the wheelchair that brought me out of the gym. My normal senses began to deteriorate, and indescribable suffering came in their place.
To this day, the most excruciating pain I have ever experienced was the 30 minutes that followed my head smashing into the gym floor of Carmichael Arena.
The intense ringing that filled my ears led me to believe my eardrums were going to rupture. Everything in the room seemed to be spinning at an inconceivable rate and being pushed in the wheelchair only exasperated this. While I was whisked away, I felt as if I was on one of those fast-spinning, gravity-defying carnival rides that you would find at the state fair — the kind of ride that makes you sick to your stomach. By this time, I was nauseous and aggressively dry heaving. My throat felt like it was closing up, and I was gasping for air. The pounding in my head was extreme; it felt like something was trying to break out from inside my skull. My eyes ached, and my vision was clouded with piercing white light. It almost felt cinematic, like a dying character being told “don’t go into the light.”
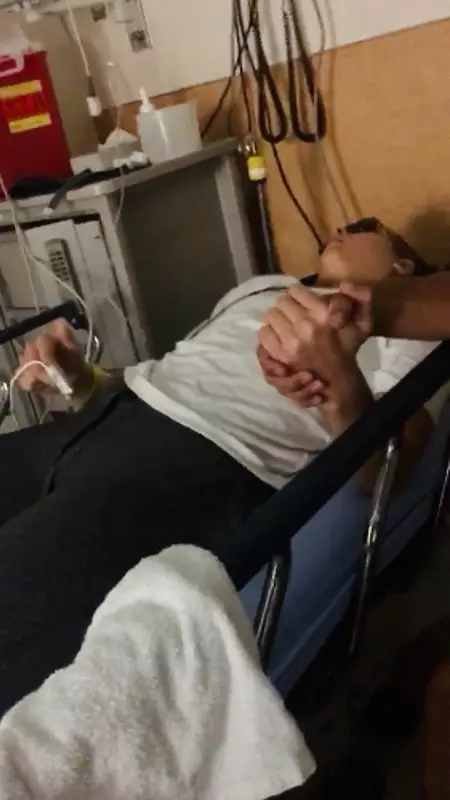
I remember experiencing all of this simultaneously, while also streaming in and out of consciousness. I even asked my trainer if I was dying. Looking back on this day, I know I overreacted, but during that 30-minute time span, death truly felt like my reality.
After those 30 minutes, my symptoms subsided; still present, but less extreme. I was brought to a doctor’s office on campus and diagnosed with my first concussion. I was clueless to concussion protocol and recovery treatment. My biggest concern was when I would be able to play again, because we were in the middle of a record-breaking season. I had to go through a series of steps and tests before I was cleared to play. My concussion symptoms — that is, after the first day — were more annoying than they were painful. They would improve each day, and after two and half weeks, I was back playing on the court. Upon returning, I thought to myself, “I’m glad it was just a concussion, and not a bad sprain or break … otherwise I’d have to be out for way longer.”
Reflecting on that now, the naiveté of this statement sickens me, and I only wish I could go back in time to share what I know now with my ignorant freshman self.
The summer going into the 2017 volleyball season, I had never felt more on top of my game. I trained all summer and was in the best shape of my life. I played some of my highest level of volleyball, all while accomplishing one of my dreams of playing for the USA Collegiate National Team. After that I headed back to work camps at UNC and prepare for what looked like a promising season. Concussions were the last thing on my mind, partly because I knew I would never make the dumb decision of launching myself airborne towards a ball again.
During the last open gym of summer, our team was scrimmaging, and I called for a fast set to the pin. I saw a wide-open seam in the block and swung. At the last second, the middle pressed her hand into the seam. The ball instantly bounced off the block, into my face, and ricocheted back over the net. My neck snapped backwards in response to the initial hit, and I landed dazed. I felt a slight headache and dizziness, but I didn’t think much of it because I was not experiencing any of the severe symptoms that accompanied my first concussion. I continued to play the rest of practice.
After open gym, I let our trainer know that I got hit pretty hard and had a bit of headache, but nothing too concerning. She gave me some ibuprofen and told me to monitor how I was feeling in the following days. After Thursday’s practice, I went home and felt fine for the rest of the night. The next day I was a little groggy and slept a lot more than usual, but for the most part I still felt normal. I did not experience severe symptoms until Saturday morning — a day and a half after the initial impact. I woke up Saturday morning dizzy with an intense headache and nausea, accompanied with light and noise sensitivity. I called our trainer and she drove over. The symptoms progressively got worse and I began to projectile vomit.
The trainer rushed me to the ER to get a CT-scan of my head because of the sudden increase of symptoms, which is often an indication of a more serious problem, like a brain bleed. Thankfully, the scan came back clear, but the doctor confirmed I was yet again concussed. What I did not know at the time was that this concussion would change the course of my life.
I was released from the hospital and prescribed anti-nausea and headache medication. I laid in a dark room for two days, and when I wasn’t asleep, I was throwing up. Around day four, my symptoms started to progressively decline. I was under the assumption that just like my first concussion, I would go through the protocol and be back in no more than two weeks. Our 16-day preseason training was a week away, and I was determined to play in the season opener at the end of the month in Wisconsin.
After a week of resting, I started feeling more normal, but I noticed that certain things or activities would trigger certain symptoms, causing them to range from barely noticeable to unbearable pain.
I began feeling more and more frustrated because I was not getting better or progressing the way I did the first time around. The symptoms became more bearable but they never went away. I convinced myself I was feeling better by creating an excuse for each of my symptoms. I told myself the headaches were just normal headaches that everyone got, the exhaustion was from not getting enough sleep, and the oversleeping was because I was exhausted — an oxymoron, I know. I fibbed my way through concussion protocol, telling the trainers what they wanted to hear so I would be cleared to play. I was cleared two practices before we competed, and fully practiced in one of them before playing the following day. During warm-ups, I began to get a bad headache. I took a couple of ibuprofen and brushed it off like it was no big deal. During the game, I got hit in the head twice while blocking. I was only a little bit concerned because neither hit was significantly hard. I slept through the night and felt OK during the morning. We took a bus to the airport and flew back to Chapel Hill. That Monday, I knew deep down that I was in fact, not OK.
I attempted to practice, but less than halfway through, I completely broke down. I was sobbing uncontrollably, and my trainer took me to a quiet, dim-lit room. I bawled until there were no more tears left to cry. My trainer comforted me and helped calm me down. She assured me things would be alright. School started, and things started to go downhill — fast.
I realized on the first day of class I was unable to read more than a sentence or two. My eyes weren’t tracking properly. When I attempted to read anything longer than a sentence, all I saw were jumbled letters. My eyes didn’t know where to look. I went to see our team physician, and she told me I wouldn’t be traveling to Puerto Rico with the team the upcoming weekend so I could focus on recovery. I had been looking forward to that trip since the release of our schedule during the spring.
On Thursday, the day before the team left for Puerto Rico, I started feeling unlike anything I had ever experienced. I was scared.
My body started shaking uncontrollably and I began to vomit. Thankfully, my roommate and friend were home, so they quickly brought me to the emergency room. I was too weak to walk, convulsing, and continuously throwing up. The doctors ran different tests, which seemed to take hours, before figuring out my sodium levels had dropped to 119. Normal sodium levels are between 135-145. Sodium levels below the 120 range commonly cause seizures, comas, and even death. Research shows concussions and brain injuries can impair the pituitary gland which regulates sodium levels. The doctors were uncertain if this was caused by my concussion or another underlying factor. However, it’s important to know how wide the spectrum of issues from a concussion can be.
The doctors hooked me up to a saline IV and I was monitored throughout the night. My coach and some teammates stayed with me at the hospital until around 1 a.m., even though they had to wake up at 4:30 a.m. to catch their flight to Puerto Rico. Their presence was a necessary comfort I desperately needed during the scariest night of my life. I will always be incredibly thankful for my Carolina family and the selflessness that was shown to me that night.

After being released from the hospital, I focused on taking my recovery process one day at a time. I knew it was going to be anything but easy. It was like riding a roller coaster that I could not get off; there would be days where it would seem like I was getting better, but then I would wake up the next morning feeling worse than ever before. Healing from my concussion was anything but linear.
Arguably, I spent more time in various doctors’ offices than I did in my own apartment.
I remember making a joke to my coach at one point, saying I was a Division I doctor-goer, because while my teammates were doing 20-plus hours of training a week, I was at one of my never-ending appointments. During this year I cried more days than I didn’t, and prior to my concussions, I think I cried maybe two times total since starting college. I medically under-loaded my class schedule, and thankfully for the classes I was still enrolled in, the professors were accommodating and more than understanding.
What’s more, the concussion caused my pre-existing ADHD to heighten, so the classes I was still in seemed unnecessarily laborious. I was put in vision therapy for the entirety of the fall semester to retrain my eyes to track. I had to start wearing special glasses that spaced letters out and helped me to see better. My academic advisor would read me the assigned readings from class when I still couldn’t read for myself.
On top of vision problems, my heart rate was affected as well. Concussions commonly affect the autonomic nervous system, which regulates all sorts of bodily functions like heart rate. While laying down, my heart rate would be in the 50s, and upon sitting up it would jump to the 90s. When I would stand, it would go into the 120s, and walking put it in the 140s. A light jog would cause my heart rate to reach the 170s. The rapid variance in my heart rate would cause me to get light-headed every time I would stand. I had to wear a heart monitor for weeks. With this cardiovascular problem, I was unable do even the simplest of workouts.
One night, a few months after suffering my concussion, I caught a 24-hour bug that was traveling around the team. This sickness caused nausea and vomiting. I woke up feeling sick, so I walked to the bathroom feeling more light-headed than normal. When I was walking back to my room, I passed out — making a loud thud from hitting the back of my head on the tile floor of my apartment. I woke up to my concerned roommate frantically talking on the phone with my trainer, asking what to do. I was groggy and confused. I went to the hospital for my second CT scan of the year to make sure my skull was intact. Thankfully it was, but unfortunately, I was set back in the recovery process and three weeks of progress in vision therapy were erased.
When sustaining my concussion, I also got whiplash. Whiplash mirrors many of the same symptoms caused by a concussion. I had X-rays taken of my neck to gage the severity of the whiplash. To this day, I will never forget the phone call I received from my doctor saying, “don’t freak out, but there is a possibility you could potentially be acutely paralyzed. You would need spinal surgery to fix your neck. Further imaging needs to be taken in order to confirm this. The next possible appointment for a neck MRI is tomorrow at 2 p.m.”
Obviously, I freaked out, imagining the worst possible scenarios and crying on and off non-stop until my appointment the next day. I had to wait three days for the results of the MRI. As you could imagine, the time in between the appointment and when I received the results moved unbearably slow. I was praying non-stop and hoping for a miracle. The MRI results showed my C3 and C4 vertebrae were congenitally fused, meaning I would not become paralyzed and I would not need spinal surgery. However, my C1 vertebrae, also known as the “atlas,” was off by 9 mm. If the atlas is displaced by as little as 3 mm, you begin to notice various symptoms. So, I saw a chiropractor multiple times a week throughout the entirety of the year to fix the alignment of my spine. The curvature of my neck was significantly changed from the impact. It has never returned to what it once was, and I still see a chiropractor frequently.
Throughout the year, I had constant and debilitating headaches. I remember the worst of these was a migraine that I rushed to the doctor’s office for. I was put on an IV and laid in agony until the medicine numbed the pain. Most days felt like a battle, and constantly fighting against life left me worn out and exhausted. I began to see my personality change right before my eyes, and I felt helpless in salvaging the person I knew myself to be. I was unrecognizable to myself and felt like a shell of the person I once was. The mental aspect of having a concussion was by far the most challenging part. I was struggling with depression and anxiety of which I have never dealt with up until that point.
The simplicity of everyday things became dreadful.
Seeing friends while walking around campus became an emotionally taxing façade. Everything I once knew about myself was stripped away. I lost my joyful personality, my identity as a student, an athlete, and as a teammate. I felt like I was letting down the people in my life because I was not the same Julia and it was obvious. The people I was closest with stuck by my side and helped me get through this arduous time. Words cannot express my gratitude for the support system I was blessed with.
Though this chapter in my life was inconceivably hard, I would not go back and change what happened to me.

I learned how to have fortitude, resiliency, and complete trust in God when facing my life’s toughest battle. Before my concussion, I used to base my faith off my worldly circumstances. But now, I realize that no matter my situation, God is still good and a relationship with Jesus is more valuable and powerful than any of life’s circumstances. My faith grew tenfold and I grew more as a person in one year than the previous 18 years of life combined.
I have a new sense of perspective that allows me to look at life through a totally different lens. I believe that no life experience is ever wasted, and if my story is able to prevent or help someone going through a similar situation, then it’s all worth it. Awareness on concussions as well as how to perceive and deal with them is necessary. In my opinion, there isn’t nearly enough awareness on the severity of concussions, due to a lack of understanding and the ambiguity that accompanies this invisible injury. Steps, like the work CLF is doing, must be taken in order to generate further awareness, and I am hoping to contribute by sharing my story.
Upon being cleared and returning to the indoor court, nothing felt the same, and I knew the sport would never feel like it once did. Even though I was cleared to play, I was still struggling with the residual effects of post-concussion syndrome. Every time I stepped on the court, I was riddled with anxiety and plagued with fear. I never did get through a full practice of indoor volleyball again. I knew something needed to change, but I refused to give up athletics.

Around this time, I had begun playing beach volleyball with the UNC club team. Beach volleyball felt entirely different than indoors to me, and far safer. To this day, I have never felt the threat of getting another concussion while playing beach. The ball is a bit bigger and softer, and the game is played a lot differently — this is not to say that getting a concussion in beach couldn’t happen, but the chances of getting one are far slimmer. Plus, I always had a dream of playing beach volleyball professionally after college, even though I’ve never actually played the sport.
This was my opportunity to change my path and pursue a dream I wouldn’t have had enough courage to, had the concussion not made the familiar now unfamiliar. So, I emailed some beach volleyball programs, telling them my story and my interest in the sport. I visited some California schools before deciding on the University of Hawai’i.

My first year at Hawai’i was challenging, but in a far different way than the previous two years of dealing with concussions. I was pushed as an athlete in ways that I’ve never experienced before. I felt like a fish out of water playing beach volleyball. I honestly hated the sport in the beginning, mainly because of the difficult and uncomfortable transition process. Beach volleyball is a game of imperfections and I strive for perfection in my sport, so it was beyond frustrating to say the least. I made a promise with myself to stick with it, regardless of how I felt.
Once competition started, I began to fall in love with beach volleyball and the tiresome hours of unenjoyable work paid off. Just like the healing process of my concussions, my progression in the sport of beach volleyball resembled that of a roller coaster. Some days I would feel giddy with excitement, loving every moment of learning and growing, while other days left me questioning the belief I had in myself and the decision I made in changing my life course to pursue this sport. What got me through the challenging times was holding onto the days where everything felt right — like I was exactly where I was supposed to be.
The good days started to multiply, and the bad days began to diminish. I am now able to look back at the trials of these past two years with clarity, making sense of their importance in shaping my life’s path and purpose.
There is a quote I came across during the time of my concussion and one that I still hold near to my heart:
“Sometimes when you’re in a dark place you think you’ve been buried, but you’ve actually been planted.”
My concussion was a chapter in the story of my life, and because of it, I’ve been planted. Rooted in faith, I continue to grow towards my dreams.
July 2020:
If you were to tell me I’d be where I’m at today in the midst of recovering from my concussions, I would have called you a liar. I remember feeling like I would never see the light at the end of the tunnel and the life that I once knew would never be able to reconstruct. The lifeline that I clung to and relied on during those tough times was my faith. And faith the size of a mustard seed can move mountains. I firmly believe faith is the reason the seemingly insurmountable mountains in my life were overturned. It’s now been 3 years since my last major concussion. Today, I’ve never felt better physically or mentally, including prior to the head traumas — which is crazy to think! I am happier, healthier, and feel more like myself than ever before. Don’t get me wrong, I still have bad days, but most days I wake up excited for what lies ahead. I recently graduated with a BA in Communications from the University of Hawaii at Manoa with a 3.55 GPA (which was shocking because I’ve always struggled academically). I will be starting a graduate program in the Marshall School of Business at the University of Southern California in the fall. I will be competing for the Trojan’s on the beach volleyball team while using the remainder of my NCAA eligibility. I’ve fallen in love with beach volleyball and plan on pursuing this passion for as far as it will take me. I never in a million years could have orchestrated or picked a better path than I am on now. It’s obvious God’s sovereign hand has been shaping every step and detail of the way. I now think about life wildly different from my previous conceptions before my concussions and that is one of the biggest blessings that came from this hardship. I will always take the lessons I’ve learned during these past few years with me wherever I may go next.
Are you or someone you know struggling with lingering concussion symptoms? We support patients and families through the CLF HelpLine, which provides personalized help to those struggling with the outcomes of brain injury. If you are seeking guidance on how to choose the right doctor, find educational resources, or have any other specific questions, we want to hear from you. Submit your request to the CLF HelpLine and a dedicated member of the Concussion Legacy Foundation team will be happy to assist you.

